Beat the heat with the summer edition of the CCA provider newsletter
Learn how to submit corrected claims, review changes to CCA’s readmission payment policy, and find out how to refer members for in-home urgent care in the summer edition of the CCA provider newsletter.
Featured News
At Commonwealth Care Alliance (CCA), we are dedicated to continuing to support our provider community, who are instrumental in providing the best possible care to the members we serve.
In recent months, CCA has heard significant concerns from our provider community in regard to the administrative burden providers are experiencing when submitting corrected claims to CCA. Effective June 1, 2021, we are pleased to announce that CCA has implemented an industry-standard process where providers can now submit their corrected claims electronically. We are in the process of updating our Provider Manual and EDI companion guides, and appropriate communication will be shared once these documents are updated. Until we update the Provider Manual and EDI companion guides, we are providing a quick reference guide on how corrected claims can be submitted electronically.
How to Submit Corrected Claims Electronically:
Resubmission (Frequency Code 7):
Only submit resubmissions for claims that have been finalized.
Submit one corrected claim for each one finalized claim.
- In Loop 2300:
- In the claim segment, field CLM05-3 needs to have a value of 7.
- In the REF segment, use qualifier F8 and put in the CCA claim number of the original submission.
Full Void (Frequency Code 8):
Only submit voids for claims that have been finalized.
Submit one void for each one finalized claim.
Only submit voids when the entire claim is to be voided.
- In Loop 2300:
- In the claim segment, field CLM05-3 needs to have a value of 8.
- In the REF segment, use qualifier F8 and put in the CCA claim number of the original submission.
If you have any questions, please contact CCA Customer Service at 800-306-0732. For EDI support, please email [email protected].
CCA is committed to providing high-quality care coordination for the members we so proudly serve. That’s why we are excited to continue growing our ancillary network. As always, it is a best practice to routinely check the CCA Provider Directory to find contracted providers in your area.
| Provider Name | Service |
| Women’s Image Center | DME |
| Collins Surgical | DME |
| First-Call Medical, Inc. | IDTF |
| Coastal Sleep Diagnostics, Inc. | Sleep |
| Alliance Neurodiagnostics, LLC | IDTF |
| Chelmsford MRI | Imaging |
| SunMed Medical Systems, LLC | DME |
| Invitae Corporation | Lab |
| CBLPath, Inc. | Lab |
| Stephen P. Tobias dba Tobias Hearing Aids, Inc. | Hearing Aids |
| New England Tissue Issue, PLLC | Lab |
| ProPath Services, LLC | Lab |
| DRUGSCAN | Lab |
| MedTox | Lab |
| Litholink | Lab |
| Revolution Charlwell, LLC | SNF |
| Sole Remedy, LLC | DME |
| Eye Health Services | Vision |
| Acupuncture Herbs and Beyond, LLC | Acupunc |
| Pure Life Renal of Stoughton, LLC | Dialysis |
| Harvmit Acupuncture | Acupunc |
| Sun Wellness Acupuncture PC | Acupunc |
| Outpatient Mobile Solutions, Inc. | OP Rehab |
| Tai Chi Acupuncture and Wellness Center | Acupunc |
| Regina Gibbons | Acupunc |
| Stern at Home Physical Therapy PC | OP Rehab |
| Wells Physical Therapy and Associates | OP Rehab |
| Capital Marketing Group, LLC, dba Holyoke Optician | Vision |
New in-Network Ancillary Contracts as of 7/2020–5/2021
CCA News & Updates
At Commonwealth Care Alliance (CCA), we are dedicated to improving care for individuals dually eligible for MassHealth and Medicare with complex medical, behavioral health, and social needs. Our mission is to provide the best possible care to the members we serve.
Following the precedent established by the Centers for Medicare and Medicaid Services, CCA recognizes that the frequency of readmissions to an acute care hospital shortly after discharge is an index for quality of care. Thus, CCA has implemented a process for reviewing such readmissions.
Effective July 1, 2021, CCA will be instituting a revised payment policy for readmissions to the same hospital or hospital system within 30 days. CCA and its affiliates will conduct post-pay readmission reviews to determine if the readmission could have been prevented due to one or more of the following conditions:
- If the readmission was medically unnecessary,
- If the readmission resulted from a premature discharge from the same hospital, or
- If the readmission was the result of circumvention of the Prospective Payment System by the same hospital.
Note: The above guidelines are only applicable for review if the member entered the same acute facility within 30 days.
For more details, please visit our website at commonwealthcarealliance.org. The Readmissions Within 30 Days policy can be found on the “For Providers” section under Policies and Guidelines: Payment Policies.
If you have any questions regarding this letter, please contact the CCA Provider Services team at 866-420-9332.
At Commonwealth Care Alliance (CCA), we’re committed to supporting our provider partners, so that together we can deliver the highest-quality, individualized care to our members. For this reason, we’ve updated our website (www.commonwealthcarealliance.org) to feature an enhanced navigation system and richer content—to help you quickly and easily find the information you need from CCA. Below we’ve outlined some of the key updates and features of our new site.
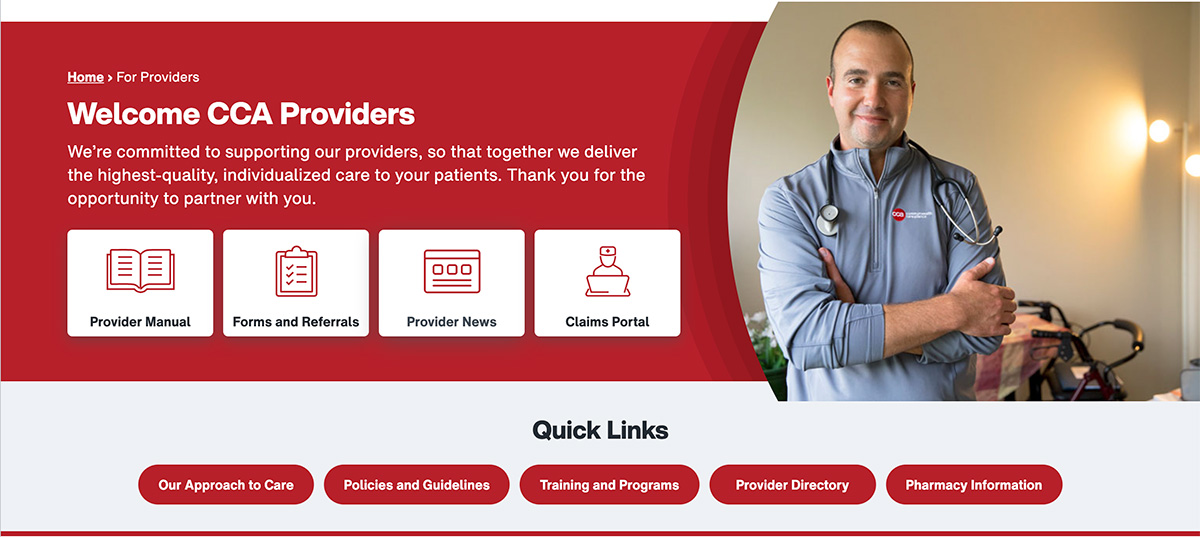
Enhanced navigation: The new site features three easy ways to find what you need:
- Four main navigation buttons located at the top of the Provider page, for easy access to our Provider Manual and other important forms and documents
- “Quick Links” that help you drill down by topic and access other key information, such as our trainings and programs
- A hamburger menu (drop-down) that helps you navigate to other sections of the site when needed
New content and improved page organization, including:
- A Provider News page that combines the latest newsletter and COVID-19 alerts from CCA
- An integrated Policies and Guidelines section that combines clinical, quality, and payment information
- Easier access to our Provider Directory and a detailed service map
For questions or support, you can contact us at 866-420-9332. As always, thank you for your continued partnership in serving CCA members.
At CCA, we are deeply committed to supporting our provider partners. We understand the importance of improving our communication and optimizing administrative tasks, so that collectively we can focus more time on delivering the highest-quality, individualized care to our members. That’s why we’re launching a portal that will offer many administrative efficiencies to our providers managing CCA members.
To launch the portal, we have partnered with HealthTrio, a leading software-as-a-service provider for the healthcare industry. We chose HealthTrio after extensive research because of the vendor’s demonstrated success and commitment to improving experiences in value-based care, data integration, care coordination, and member and provider engagement.
The new CCA Provider Portal will act as a self-service single location allowing you to quickly and easily access important member information and complete critical tasks—in real time. As part of the phase one launch of the portal, you will be able to:
- Verify member eligibility
- View member authorizations
- Send credentialing information
- Connect with CCA via HIPAA-compliant secure messaging at your convenience
- Receive and manage electronic CCA provider communications
- View remittance advice/explanation of payment
- View member roster reports
- Manage office staff’s access to the portal
By using the portal, you will have the flexibility to manage many of these tasks while reducing wait time. Moving forward, CCA plans to continuously update the features of our portal and will keep our provider community updated on future releases.
Next Steps
In the coming weeks, CCA will send you more information on when the provider portal will go live and how to register.
For questions about the provider portal, you can contact us at 866-420-9332. As always, thank you for your continued partnership in serving CCA members.
Guidelines & Tips
As a Commonwealth Care Alliance (CCA) contracted provider, you have an obligation to coordinate members’ care with contracted, in-network providers. This includes all services, such as laboratory, durable medical equipment, radiology, behavioral health providers, skilled nursing facilities, long-term support services, and many other specialties.
Before you establish a referral relationship with a provider, please take a moment to confirm that the provider in question currently participates in the CCA network. Please also confirm that the provider currently participates with your patient’s plan, such as Senior Care Options or One Care.
There are two ways to confirm in-network status:
- Check providers’ participation status on the Advanced Search of the CCA Provider Directory, found here: https://provider-directory.commonwealthcarealliance.org/Form/Index
- Contact the CCA Provider Services Team at 1-866-420-9332
Your cooperation in referring to in-network providers is greatly appreciated. This practice will promote excellent care coordination with high-quality, CCA providers who care and provide services for CCA members.
The Standard Prior Authorization form is required for all prior authorization submissions. It should be submitted prior to delivering services to the member. You can find the form here: https://www.commonwealthcarealliance.org/ma/providers/forms-and-referrals/
Required Information for Processing Authorizations
- All required fields on the PA form (marked with an asterisk *) are necessary for processing requests in a timely manner. Not including required information can cause delays in processing or denials.
- The specific information below is frequently missed on requests, which causes delays and incorrect denials. Please make sure to include this information as well as all other required information.
- Servicing facility represents the location where the requested services will take place. It is not sufficient to only list the Servicing Provider’s information—we also need the location where they will perform the services.
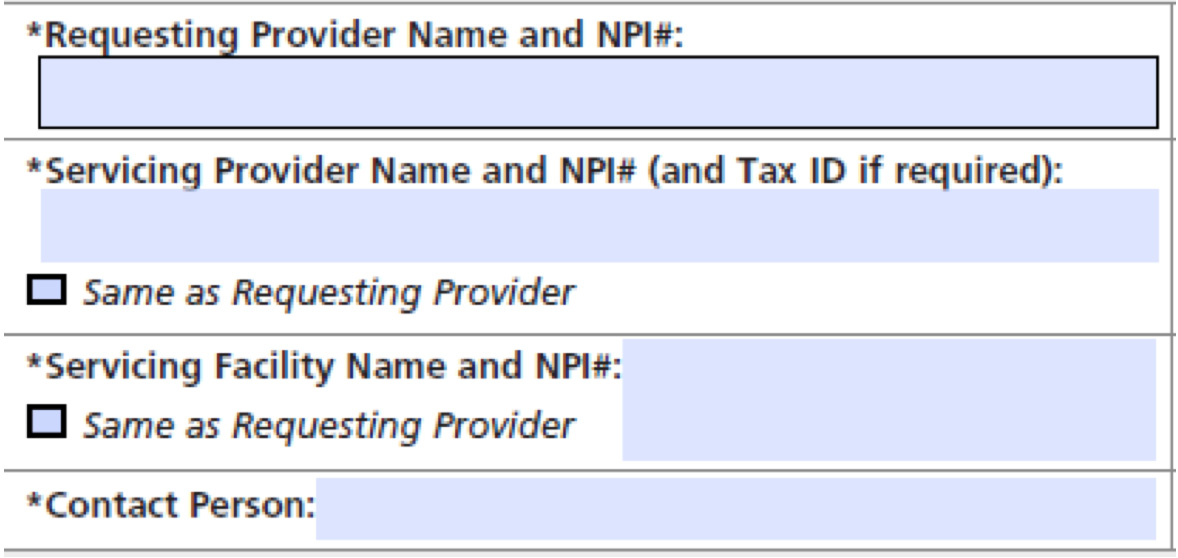
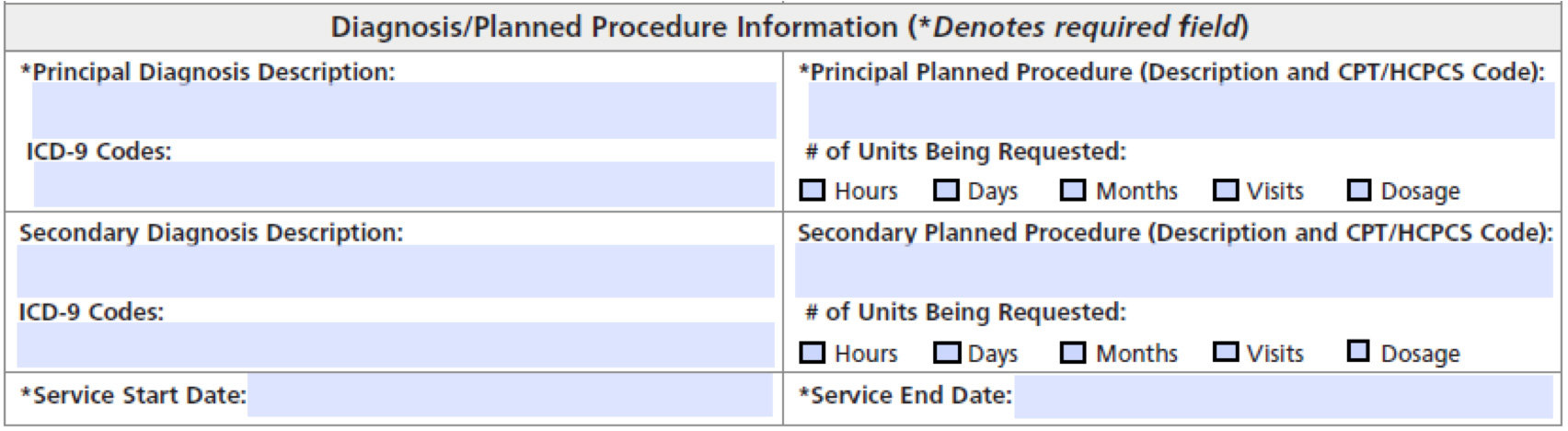
- Diagnosis & CPT/HCPCS codes
- – CPT/HCPCS codes and description of services
- – The frequency and number of units for each code
- – The dates of service
- – ICD-10 diagnostic codes
- Clinical documentation to justify the requested services must be attached when submitting a PA form. This includes office notes and any written/MD orders. Lack of supporting clinical information delays the decision and your ability to provide the requested service.
- Servicing facility represents the location where the requested services will take place. It is not sufficient to only list the Servicing Provider’s information—we also need the location where they will perform the services.
Submission of Duplicate PA Requests
PA requests should be submitted only once, unless there is an update. Please do not submit a duplicate request if you are waiting on a decision. Authorizations are processed within regulatory timeframes (please see the FAQ on Authorization Requests located at the link provided at the top of this page). If you are looking for the status of a PA request that you have submitted, please contact CCA Provider Services at 866-420-9332.
Expedited PA Requests
Expedited requests should only be made when waiting for the decision under the standard time frame could place the member’s life, health, or ability to regain maximum function in serious jeopardy.
It is estimated that as much as 67% of all emergency department visits are avoidable.* CCA’s instED® program helps ease this burdensome statistic, allowing our members to receive the urgent medical care they need in the comfort of their own home.
instED is a reliable resource that fills the gap between primary care and emergency care—even for those with significant health needs. With instED, you’ll have peace of mind knowing your patients are cared for by highly trained paramedics, and that you’ll be kept informed of the care they receive.
How to Request an instED Visit
It’s quick and easy for providers and patients to request an instED visit.
Go to www.instED.us1 or call 1-833-9-INSTED (1-833-946-7833).
instED visits are free of charge for CCA plan members.
For more information, please contact [email protected].
* Stanton, M. W., & Rutherford, M. K. (2005). The high concentration of U.S. health care expenditures. Agency for Healthcare Research and Quality, 19, 06-0060. Retrieved from http://archive.ahrq.gov/research/findings/factsheets/ costs/expriach/
The instED program is not available in all areas. Other in-home urgent care providers are available in the CCA network. For any life-threatening conditions or medical issues that need immediate attention, call 911.
Commonwealth Care Alliance recognizes that while pregnancy is a special time for families, it can also bring challenges. This is especially true for CCA members who are at increased risk due to physical or psychological health conditions and social determinants of health.
Research shows that doulas improve birth outcomes, and CCA recognized the benefit of offering doula care through our member-facing Health Outreach Workers, who deliver culturally and linguistically competent support. Our community-based doulas receive specialized training through DONA International, the leading doula certification organization in the world.
The CCA doula program provides specialized support to members throughout the perinatal period, including pregnancy, labor, and birth, and up to one year postpartum.
What does the doula offer?
Doulas do not provide medical care or advice, but they do offer many valuable benefits:
Physical and Emotional Support
Doulas understand the changes that happen during pregnancy. They will suggest comfort measures before, during, and after birth. Doulas encourage and support parents with information on a range of topics including preparing for labor and birth, self-care, breastfeeding, and infant care.
Evidence-Based Information and Decision Support
Doulas are trained to understand what families need. The doula offers reliable information so moms and families can make informed choices about the birth and the baby.
The doula can facilitate communication between the member and her obstetric care providers to foster understanding and trust.
Please keep this program in mind for your pregnant patients who are CCA members and refer them to their care partner for more information or to enroll.
You can find key resources to support CCA members in our updated Provider Manual. This includes an up-to-date contact list available online. View the Provider Manual Contact List.
Keeping your information up to date in our Provider Directory helps your practice by making it easier for our members to find accurate information about your practice locations. Updating your information in our health plan provider directories also helps our members:
- Get easy access to your services
- Receive important information about your practice
Your Assistance Is Greatly Appreciated!
If you wish to provide your updated information to CCA, please email us at [email protected].
Learn more about the CMS Provider Directory regulations on our website here.
Have a colleague you think would be interested in subscribing to CCA Provider News?
More information about the quarterly provider e-newsletter.
Sign up to receive the newsletter.
1 When you click this link, you will leave the Commonwealth Care Alliance website.